Health
/ArcaMax

For years, she raised alarms about her apartment. When the city finally acted, she ended up homeless
LOS ANGELES -- As she stuffed her clothes and papers into a suitcase and prepared to walk out the door of 5700 S. Hoover St. for the last time, Daviell McKinley had no idea where she would live.
She'd been complaining about living conditions at the residential complex for years, writing increasingly desperate messages to city officials to try ...Read more

Ex-etiquette: Putting kids first on Halloween
Q. Halloween is always a problem. I want the kids to be with me and their dad wants them to be with him. I keep trying to tell him that the kids want to trick-or-treat with their friends, not in a neighborhood 30 minutes away, but he says they have friends near him, too. It’s so frustrating! Their dad never listens to me. What’s good ex-...Read more

No strings on me: What the Sugar Hole puppets have learned about human nature
CHICAGO -- The Sugar Hole puppets are an odd bunch. Since May they have appeared every Saturday and Sunday and offered passersby cones of ice cream. When the weather turned, they began serving soup, hand pies, beer and wine. They are not pushy. They are plush. They poke their heads out of a warren on Hamlin Avenue and take orders, then retreat ...Read more

Heidi Stevens: A thank you note to my 40s, which are now in the rearview mirror
This is a thank you note to my 40s, which I just left behind.
My 30s gave me my children. My 40s gave me the setbacks and screwups and strength and soul-searching to be worthy of them.
My 30s gave me some of my closest friends. My 40s gave me the chance to lean on them and the privilege of being leaned on by them. Some of us (me) took a while ...Read more

'Stay in that loneliness:' In Chicago, monks study, work and pray seeking God
CHICAGO -- A siren screamed down 31st Street as six men faced one another in a dim church and began to chant.
They chanted standing up. They chanted bent over. Above a thumping bass from a passing car, they prayed to the holy trinity through St. Benedict that travelers would arrive at their destinations and for seasonable weather. They prayed �...Read more
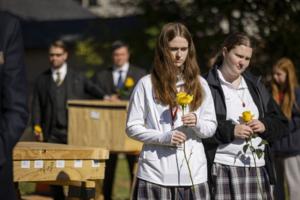
101 indigent, unknown people buried with dozens of strangers there to mourn them; 'We're going to walk that last walk with them'
CHICAGO -- When 101 people were laid to rest at Chicago's Mount Olivet Cemetery last Wednesday afternoon, no family or friends were there to mourn them. Yet they were certainly not alone.
As cold sunshine flooded the cemetery, around 20 Catholic high school students stood sentinel in their uniforms by the wooden caskets, holding yellow roses ...Read more

On Gardening: Unplugged salvia group grows to four in 2025
The Unplugged salvia group is growing to four in 2025 and that can be your start to an epic red, white and blue garden. There is also an Unplugged Pink that has 26 awards in the trophy case. Unplugged So Blue and Unplugged Pink have won a whopping 63 awards in what seems to be just a couple of years. Plus, what I am seeing in my own garden makes...Read more

Sea lions are driving La Jolla into a frenzy. Other beach towns might be next
LA JOLLA, Calif. -- La Jolla’s coastline is being conquered.
Its colonizers have made their home in the seaside neighborhood’s rocks, terraces, beaches and caves. They make their presence known by barking and wailing all day and night. And they absolutely reek.
They’re sea lions — and they’re here to stay.
Unlike harbor seals, which...Read more

Ask Anna: Forget red flags -- here are 5 green flags of a supportive partner
Dear Anna,
I'm a 41-year-old woman, just getting back into dating after an eight-year relationship, which ended a little over a year ago. In the past, I’ve spent so much energy looking out for red flags that I realize I’ve never really paid attention to the good signs — the green flags. As I’m starting to date again, I want to approach ...Read more

All in the family: This school has 10 sets of brothers playing football
LOS ANGELES -- Oh, brother.
Happening at Hart High in Los Angeles is a sports anomaly for the record books. Within the varsity and junior varsity football programs are 10 sets of brothers.
"Isn't that crazy?" said Kimme Frithsmith, mother of varsity starters Ryder and Matix Frithsmith.
That's 10 families contributing 21 boys to playing ...Read more

Erika Ettin: Feeling stuck in dating
A few years ago, I received this emotional question from a former client. I appreciated how she allowed herself to express her feelings in such a raw manner and thought it might be applicable to other readers.
“I’m really struggling with my love life lately. Over the weekend, my family got together for my mom’s birthday, and both of my ...Read more

Why a Sacramento nonprofit is buying homes, empty lots in city's underserved neighborhoods
SACRAMENTO, Calif. — North Sacramento homeowner Robin Moore was waging a 16-year battle against tall weeds and trash on a vacant lot next to her house when she was seized by a vision for the plot of land.
Gone were the garbage and invasive plants. In their stead, she pictured a tiny orchard and garden beds bursting with fruits and vegetables ...Read more

Kids are sucking down baby food pouches at record rates. 'We're going to pay for it,' experts say
LOS ANGELES -- Every week, Caitlin Scuttio stops by Target and piles her cart with pureed food pouches for her 4-year-old and twin 18-month-olds sons.
In goes a 24-pack of unsweetened applesauce. Then a 24-pack of the fruit and veggie blend. And finally, the yogurt pouches for her oldest son's breakfast. "He'd eat six apple sauce pouches a day ...Read more

Ex-etiquette: Bonus daughter
Q. My bonus daughter and I get along very well and many people who meet us just assume I am her mother. I believe I should always support her mother, so I am quick to correct the assumption. Even though she has never said anything, I can tell by my bonus daughter’s expression that she is disappointed by my clarification. Is it necessary to ...Read more

The Kid Whisperer: How to get great classroom behavior without using a behavior system
Dear Kid Whisperer,
I attended your Behavioral Leadership training two years ago and have found many great successes with your strategies in my classroom.
I used to use a system for tracking kind acts in the classroom and using class-wide rewards, and I’m thinking about returning to a similar one that I saw on Facebook. The goal is to keep ...Read more

What exactly's going on with 23andMe?
23andMe is facing scrutiny, with some experts calling it the beginning of the end for the popular genetic testing company. It's been a rocky year for the saliva-based DNA testing brand, including a high-profile data breach and resignations from the company's board last month.
Users are wondering what's next — and if their personal data (...Read more

A TikToker's Florida home flooded 3 times in 4 years. Now, she's raising it by 12 feet
ST. PETERSBURG, Fla. -- Exhausted, though relieved to have survived, is how Dr. Meghan Martin summarized her Hurricane Milton experience in her first post-storm update to her more than 2 million TikTok followers last week.
“These hurricanes, man, like, back to back like this,” she said as she ruffled her short, wavy hair and exhaled.
The ...Read more

A tale of two turfs: Bay Area residents split over using artificial grass
SAN JOSE, Calif. — Summer may be over, but there’s a hot debate brewing that’s becoming more intense and thought provoking by the day, and it’s all about — grass?
Yes, grass. As school districts look to resurface their athletic fields and cities consider how to update public parks, local leaders must decide what kind of play surface ...Read more

Navigating this world-record corn maze is a test of the human psyche
DIXON, Calif. — Deep inside one of the world's largest corn mazes, where the tri-tip sandwiches and soft-serve ice cream purchased at the concession stand have become but a memory and all that can be seen in any direction are dirt paths and dead-end walls of green plants whispering in the breeze, people tend to reveal themselves.
From humble...Read more

Heidi Stevens: Saying goodbye to a childhood house that was so much more than a house
Maybe it’s because my best friend and her sisters just helped their parents empty and sell the house they (we) grew up in.
The house where we baked cookies and figured out makeup (kind of) and celebrated birthdays and talked about boys and got in some trouble and made some amends and hosted wedding showers and nursed our babies and grieved ...Read more
Popular Stories
- Heidi Stevens: A thank you note to my 40s, which are now in the rearview mirror
- 101 indigent, unknown people buried with dozens of strangers there to mourn them; 'We're going to walk that last walk with them'
- On Gardening: Unplugged salvia group grows to four in 2025
- Kids are sucking down baby food pouches at record rates. 'We're going to pay for it,' experts say
- No strings on me: What the Sugar Hole puppets have learned about human nature






















