Wearable glucose monitors offer real-time data, but for healthy people no guidelines exist to interpret the numbers
Published in Health & Fitness
Keeping tabs on blood sugar throughout the day used to be the exclusive domain of people with diabetes. But in 2026, anyone can buy a user-friendly wearable device that provides minute-by-minute readouts on how their glucose levels respond to food and movement.
These glucose numbers are increasingly being tracked by people who are healthy but want to lose weight or optimize their wellness.
I am a behavioral scientist who has spent the past decade studying how real-time data captured through wearable sensors and mobile technologies can help promote a healthier lifestyle. I’ve found that for people who don’t have diabetes, using such a device for a few weeks can bring insight into how their body reacts to their eating patterns and daily habits.
But researchers still don’t know how these fluctuations affect health for people who don’t have diabetes. In the absence of meaningful metrics for interpreting these numbers, monitoring a constant stream of data doesn’t directly help people make health-related decisions and can lead to confusion and needless anxiety.
Glucose is a type of sugar that circulates in the bloodstream after being absorbed from food. It is the body’s primary source of energy.
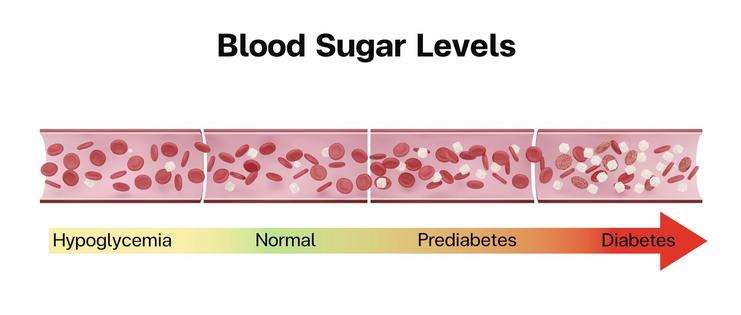
For people without diabetes, glucose levels generally stay in the range of 70-120 milligrams per deciliter (mg/dL) of blood throughout the day. After eating or drinking, levels could exceed 140 mg/dL but should come down to the normal range within a couple of hours. That’s because the pancreas responds to a glucose spike by releasing a hormone called insulin, which brings the glucose number down.
Muscles burn glucose for fuel, so physical activity also helps normalize glucose levels.
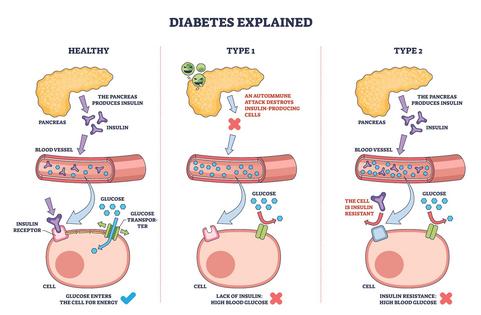
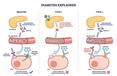
Glucose levels generally run high with diabetes. People with Type 1 diabetes, whose bodies don’t make enough insulin, rely on glucose numbers to tell them when to take a dose of insulin. People with Type 2 diabetes use the numbers to monitor the effect of their medications and lifestyle changes and to get a fuller picture of their glucose control.
Devices that track glucose numbers have been around since the early 1970s. Early versions consisted of test strips that detected glucose levels in urine. Finger prick tests, or glucometers, which were developed in the 1980s, are still used by some people today and measure them more directly by applying a tiny blood drop to a test strip.
To make the technology more convenient, companies in the early 2000s developed continuous monitoring devices that consist of tiny sensors inserted just under the skin that detect glucose in fluid that surrounds cells. Initially, these devices could give readings every 15 minutes for several days at a time, but recent versions sample more frequently.
Today, the technology has evolved even further. The most advanced glucose monitors under development come in the form of watches or rings with noninvasive sensors that use light-based techniques to detect glucose in body fluids. Many also rely on machine learning to provide more accurate readings by detecting each person’s unique physiological patterns over time.
For decades, continuous glucose monitors were available only with a doctor’s prescription. But in March 2024, the Food and Drug Administration approved the first over-the-counter continuous glucose monitor in the U.S., making them widely accessible.
There’s no doubt that continuous glucose monitors are a game-changer. People living with diabetes rely on these devices to track what percentage of the day their blood glucose stays within healthy limits – a measure called “time in range.” Patients make decisions about managing their condition - for example, when to take insulin – on guidelines developed by researchers and physicians based on that measure.
According to a 2026 report from the Centers for Disease Control and Prevention, almost 11 million adults who have diabetes – more than 1 in 4 adults with the condition – are undiagnosed. Type 2 diabetes can develop slowly and silently, often with no noticeable symptoms for years except glucose levels that remain elevated for a majority of the day, including when people are sleeping. Tracking glucose levels might offer clues that glucose is elevated.
Tracking glucose levels may also benefit the 115.2 million Americans – 43.5% of all U.S. adults – who have a condition called prediabetes. Prediabetes is when a person’s metabolic system shows early warning signs of diabetes but they don’t have the full-blown disease.
Prediabetes generally has no noticeable symptoms, but it is reversible – meaning, it’s possible to shift your glucose levels back into a healthy range. Tracking your glucose number can reveal how diet and exercise affect it. Observing how a soda spikes your glucose levels, for example, might give you pause before you drink one next time.
Increasingly, though, people who use continuous glucose monitor aren’t diabetic – or even prediabetic. Instead, they want to understand how their bodies react to activities in their daily lives.
Diet, exercise and other lifestyle behaviors have long-term effects on health. Weight loss, for example, happens slowly. Changes in blood glucose, on the other hand, are more immediate. Tracking glucose levels thus offers real-time feedback on how your body responds to the food you just ate or the workout you just finished.
In studies I’ve conducted with colleagues, many people have found this information powerful. They were surprised to learn that eating certain foods – sugary soda, or even something healthy like a banana – causes their glucose levels to spike.
One study participant told us that seeing their real-time glucose numbers led them to make more intentional dietary choices, such as cutting back on snacking. “I’m more aware and I’m making the changes,” they explained. Another participant also noted behavior changes prompted by continuous glucose monitoring, such as trying to avoid eating so late in the evening and consuming only half a fast-food meal.
That initial wow factor – and its capacity to motivate people to make healthy lifestyle changes – may be valuable. But it’s not clear how long these changes last, or how exactly people should respond to fluctuations in their glucose number to decrease their diabetes risk or to address other health issues.
Unlike the time in range guidelines for diabetes, there is no clear framework for what daily glucose patterns are abnormal in people who don’t have diabetes – or what patterns may indicate future disease risks.
Researchers like me and my team are exploring exactly these questions.
Building a dynamic picture of how glucose levels fluctuate throughout the day in people without diabetes may point to early indicators for various chronic diseases. For example, my colleague and I recently developed a mathematical model to examine how monitoring glucose levels during sleep might help predict the risk of metabolic diseases – such as Type 2 diabetes, heart disease or fatty liver disease – in people with and without diabetes.
Additionally, continuous glucose data may reveal how people’s bodies might react differently to the same food, workout or other activity. Understanding how each person’s biology responds to the choices they make throughout the day could eventually lead to a more personalized approach to lifestyle changes that can help people maintain their health.
This article is republished from The Conversation, a nonprofit, independent news organization bringing you facts and trustworthy analysis to help you make sense of our complex world. It was written by: Liao Yue, University of Texas at Arlington
Read more:
Health apps track vital health stats for millions of people, but doctors aren’t using the data – here’s how it could reduce costs and patient outcomes
Wearable fitness devices deliver early warning of possible COVID‑19 infection
Insulin was discovered 100 years ago – but it took a lot more than one scientific breakthrough to get a diabetes treatment to patients
Liao Yue receives funding from the American Institute for Cancer Research, the American Heart Association, the Cancer Prevention & Research Institute of Texas and the Texas Higher Education Coordinating Board.











Comments