Warmer temps bring soaring tick populations – here’s how to stay safe from Lyme disease
Published in Health & Fitness
Spring’s warmer weather lures people outdoors – and into possible contact with ticks that spread Lyme disease.
Already, the 2026 tick season is booming. On April 23, the Centers for Disease Control and Prevention warned that emergency room visits due to tick bites are at their highest level since 2017. That may portend an especially severe season for Lyme disease and other tick-borne illnesses.
State health departments reported more than 89,000 cases of Lyme disease in 2023, the last year for which data is available. But public health experts believe that close to 500,000 people in the U.S. get Lyme disease every year.
As an infectious disease doctor with experience treating some of this infection’s long-term outcomes, I know that Lyme disease can be tricky because people often don’t notice tick bites and may overlook early symptoms of an infection. But left untreated, the infection can cause serious lingering – and even permanent – health issues.
Here’s what you need to know about Lyme disease to stay safe this season:
Lyme disease, named after the Connecticut town where the disease was first identified in 1975, is caused by a group of bacteria called Borrelia – most often, the species Borrelia burgdorferi.
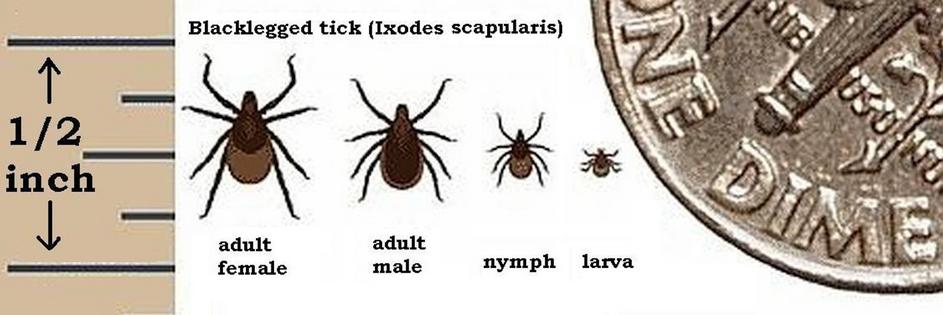
Deer ticks – also called black-legged ticks, and members of a group called Ixodes – transmit the disease after feeding on an infected animal, usually a bird, mouse or deer. When they then bite a person, they can transmit the bacteria into the person’s bloodstream.
Usually, the tick must attach for 24-48 hours to transmit the bacteria causing Lyme disease.
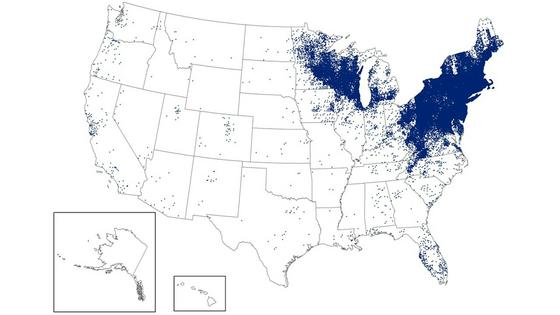
Lyme disease can occur in most regions where deer ticks live.
These ticks are most active in late spring, summer and fall – usually April to November in most regions. They emerge when the temperature is above freezing. In years when winter is shorter, ticks can emerge earlier. And they may be active year-round in regions where freezing temperatures are rare.
Approximately 90% of U.S. cases are reported from states in the Northeast, mid-Atlantic from Virginia to eastern Canada, and Upper Midwest regions including Wisconsin, Michigan and Minnesota. A few cases occasionally pop up in California, Oregon and Washington.
Since 1995, the incidence of Lyme disease in the U.S. has almost doubled.
Warmer weather and changes in rainfall patterns now allow ticks to survive in new regions of the country – and for longer periods. But even in regions where ticks lived before, Lyme disease has become more common due to increases in deer populations. As woodland areas are increasingly being developed, it may be bringing the habitat of deer and mice closer to people, increasing the risk of transmission.
Early symptoms of Lyme disease – fever, muscle aches and fatigue – generally emerge within three to 30 days after a tick bite. Another classic symptom in the first month is a target or bull’s eye rash at the site of tick bite, which occurs in about 70% to 80% of cases.
Other rashes following a tick bite can also occur. Some may be due to irritation from the bite, and not necessarily an infection.
If you know you’ve had a tick bite and experience flu-like symptoms – or if you see a bull’s-eye rash, whether you know you were bitten or not – it’s important to check with your healthcare provider about whether you should be treated with antibiotics.
A blood test for antibodies can help confirm the infection, but it can sometimes yield a false negative result, particularly in the first couple of weeks of the disease.
In most people, the rash goes away on its own. However, treatment may shorten its duration and is important for preventing other symptoms. A two- to four-week course of antibiotics can generally treat Lyme disease. Severe cases might require intravenous antibiotics.
A promising new vaccine for Lyme disease is currently being tested. In March 2026, Pfizer, the pharmaceutical company developing it, announced that in a late-stage study, the vaccine prevented the disease in 70% of people who received it.
If left untreated, the bacteria that causes Lyme can spread, potentially causing longer-term symptoms. About 60% of people who get Lyme disease and don’t treat it can develop arthritis.
In rare cases, Lyme disease can also affect the heart and the nervous system. Inflammation in the brain or the tissues surrounding it, called meninges, can cause headaches and neck pain, as well as balance issues and memory and behavior changes. It can also cause nerve damage that results in numbness, tingling and muscle weakness.
These symptoms can appear right away or much later – sometimes months to years after infection. And in cases where the disease wasn’t promptly treated, late-stage symptoms can linger even after antibiotics kill the bacteria.
Scientists don’t fully understand why, but one intriguing study found that some particles from the bacteria’s cell wall leak into the joints and can persist after treatment, spurring ongoing inflammation and arthritis symptoms.
Another reason for Lyme’s long-term effects is that it can trigger autoimmune disease, which is when the immune system attacks its own cells. What’s more, because the nervous system may be particularly sensitive to damage caused by the bacteria and related inflammation, it may take an especially long time to heal. In some situations, the damage could be permanent.
Until a vaccine becomes available, there are steps you and your family can take to help protect against Lyme disease:
Use tick and insect repellents such as DEET and picaridin, which can be applied to skin, and permethrin, which is sprayed onto clothing, to keep ticks at bay. Treating clothing with permethrin may be especially beneficial, since the substance withstands several washes.
Wear long-sleeve shirts and pants while you are gardening, hiking or walking through grass or woods to prevent tick bites. Wearing light-colored clothes makes ticks more visible, and tucking your pants into your socks can also prevent the little buggers from traveling from your pants, shoes and socks onto your legs.
Remove your outdoor clothes immediately. Washing and drying clothes at high temperature can help kill any ticks that managed to hitch a ride. And a quick shower immediately after spending time outdoors can wash ticks off the skin before they have a chance to attach.
If you spend time outdoors, perform daily tick checks, paying special attention to warm areas like your armpits, neck, ears and underwear line. If you find a tick attached, pull it off with tweezers, holding them perpendicular to the skin.
If you find a tick that may have been on the skin for more than 36 hours, ask your healthcare provider whether a dose of preventive antibiotics – generally given within 72 hours of the bite – would be appropriate.
This article is republished from The Conversation, a nonprofit, independent news organization bringing you facts and trustworthy analysis to help you make sense of our complex world. It was written by: Lakshmi Chauhan, University of Colorado Anschutz Medical Campus
Read more:
A red meat allergy from tick bites is spreading – and the lone star tick isn’t the only alpha‑gal carrier to worry about
A lab‑stage mRNA vaccine targeting ticks may offer protection against Lyme and other tick‑borne diseases
Ticks carry decades of history in each troublesome bite
Lakshmi Chauhan receives funding from NIH.













Comments