Senior Living
/Health

3 medical routines that older people may not need
Enough time had passed since the patient’s previous colonoscopy that she met the criteria to undergo another, said Steven Itzkowitz, a gastroenterologist at the Icahn School of Medicine at Mount Sinai in New York.
She was in “reasonably good health,” and the risks of the procedure — bleeding, reaction to anesthesia, perforation of her ...Read more

Study: Taking a daily multivitamin may slow down biological aging
LONDON — Taking a daily multivitamin may slow down biological aging, a study has suggested.
Experts calculated that two years of daily vitamins cut biological aging by about four months on average.
Biological aging refers to how old the body is in terms of health and function rather than the number of years a person has lived.
Previous ...Read more

‘A nightmare to think about.’ Driving behavior may be early warning sign of dementia
FORT LAUDERDALE, Fla. -- When the red light turned green, Christine Burger found herself unsure what to do next.
Burger, 73, had driven the streets of Delray Beach for many years, and had traveled often through the intersection where she was now stopped. Yet she was unsure which direction to take.
It wasn’t the first time.
“There are ...Read more

'A nightmare to think about.' Driving behavior may be early warning sign of dementia
FORT LAUDERDALE, Fla. -- When the red light turned green, Christine Burger found herself unsure what to do next.
Burger, 73, had driven the streets of Delray Beach for many years, and had traveled often through the intersection where she was now stopped. Yet she was unsure which direction to take.
It wasn’t the first time.
“There are ...Read more
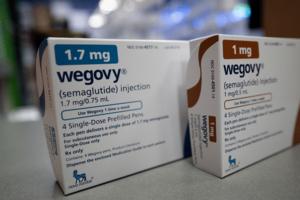
A new Medicare option for weight loss drugs: What older Americans should know
Starting in July, Medicare beneficiaries may be able to get a GLP-1 prescription for weight loss for $50 a month. It’s a notable shift for Medicare, which has long been barred from covering weight loss treatments.
The drugs, such as Wegovy and Zepbound, are effective but can be expensive without insurance coverage. They’re available in ...Read more
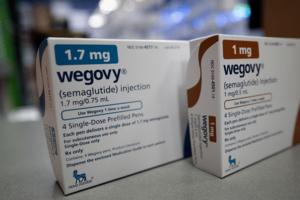
A new Medicare option for weight loss drugs: What older Americans should know
Starting in July, Medicare beneficiaries may be able to get a GLP-1 prescription for weight loss for $50 a month. It’s a notable shift for Medicare, which has long been barred from covering weight loss treatments.
The drugs, such as Wegovy and Zepbound, are effective but can be expensive without insurance coverage. They’re available in ...Read more

This 75-year-old has worked at Temple for 44 years. On Wednesday, she graduated
PHILADELPHIA — At age 75, Peggy E. Moore officially became “Temple Made” on Wednesday.
That’s what the university calls its graduates, and Moore collected her bachelor’s degree in general studies during this week’s commencement.
But Moore’s history with the North Philadelphia-based university is much longer than that of the ...Read more

Travel Trending with Kathy Witt: Exploring Japan aboard Holland America’s Volendam
Stepping aboard Holland America Line’s Volendam in Taipei, Taiwan, felt less like joining a cruise and more like slipping into a story already in motion. The 2026 Grand World Voyage had been underway for weeks by the time I arrived in early April for my 10-day Japan segment, which concluded in Tokyo. But with both passengers and crew greeting ...Read more

Streets not ready for the Bay Area’s fast growing population — seniors
SAN JOSE, Calif. -- Melissa Quilter has quit crossing the intersection of The Alameda and Marin Avenue in Berkeley when she’s walking her dog.
“My dog is older. I’m older. We don’t take risks anymore,” said Quilter, 66, who has been living by the intersection for 27 years. Without a protected left-turn signal, drivers can turn through...Read more
The help that many older Americans need most
On a recent Monday, Sandy Guzman, a community health worker in rural Oregon, drove to visit a patient in her 60s in a small city called The Dalles.
The patient lived alone, and “really struggles with social isolation,” Guzman said. After a serious fall and subsequent surgery, the woman was using a wheelchair. She confided that she would ...Read more
Hand-stitched memory bears help grieving maker and recipients
PITTSBURGH — Shirley Whitlinger knows all too well the profound, existential loneliness that follows a spouse’s death.
When David, her husband of 50 years, died from prostate cancer in 2021, after two years of chemotherapy and trials at Hillman Cancer Center, it was almost impossible not to lose herself in grief.
The couple had spent ...Read more

Trump touts 'golden age' for seniors in the friendly territory of The Villages
THE VILLAGES, Fla. — President Donald Trump came to the friendly territory of Florida’s retirement haven Friday for his first public event since an alleged assassination attempt against him, touting tax cuts for seniors and parading Dr. Phil on stage.
Trump quipped he wasn’t afraid for his safety at The Villages, a GOP stronghold where he...Read more
Hand-stitched memory bears help grieving maker and recipients
PITTSBURGH — Shirley Whitlinger knows all too well the profound, existential loneliness that follows a spouse’s death.
When David, her husband of 50 years, died from prostate cancer in 2021, after two years of chemotherapy and trials at Hillman Cancer Center, it was almost impossible not to lose herself in grief.
The couple had spent ...Read more

105-year-old Chicago woman finds herself on century-old Irish census: ‘Those years went by so fast’
CHICAGO — One hundred years ago, a few thousand miles away across the Atlantic, a quiet moment in history rippled across northwestern Europe.
The day was April 18, 1926. Ireland was coming off centuries of British rule and a bloody civil war and hadn’t paused to understand where it stood, or how it had changed, in years. But the young ...Read more

105-year-old Chicago woman finds herself on century-old Irish census: 'Those years went by so fast'
CHICAGO — One hundred years ago, a few thousand miles away across the Atlantic, a quiet moment in history rippled across northwestern Europe.
The day was April 18, 1926. Ireland was coming off centuries of British rule and a bloody civil war and hadn’t paused to understand where it stood, or how it had changed, in years. But the young ...Read more

For many patients leaving the ICU, the struggle has only just begun
The accident happened in Pittsburgh on Nov. 16. Joseph Masterson, a lawyer who was just days from retiring at age 63, suffered cardiac arrest while driving, plowed into a guardrail, and lost consciousness.
Other drivers stopped, broke the car window, and pulled him to safety. A passing volunteer firefighter performed CPR until an ambulance ...Read more

For many patients leaving the ICU, the struggle has only just begun
The accident happened in Pittsburgh on Nov. 16. Joseph Masterson, a lawyer who was just days from retiring at age 63, suffered cardiac arrest while driving, plowed into a guardrail, and lost consciousness.
Other drivers stopped, broke the car window, and pulled him to safety. A passing volunteer firefighter performed CPR until an ambulance ...Read more

Mortgages for retirees and older adults
We often think of homebuyers as young people — newlyweds and couples with small children — but baby boomers actually make up the majority of those buying a home in the U.S. Still, according to recent studies, older adults face higher rejection rates for home lending products than younger borrowers. If you’re looking to secure a mortgage or...Read more

Is it bad to spoil my grandchildren?
LONDON — Showering your grandchildren with gifts and treats comes from a place of love and excitement, but what impact could this type of spoiling have in the long term?
We spoke to Counselling Directory member Annabelle Hird, a BACP-registered counselor who specializes in supporting parents and carers, who explained why overindulging ...Read more

Seniors face unfair rents and homelessness. They need rent control
From mobile home parks in Maine to modest apartments in California, seniors desperately need rent control to protect themselves against skyrocketing rents charged by predatory landlords. Our grandparents, parents, aunts, and uncles, many of whom live on fixed incomes, face serious, life-altering consequences if politicians don’t protect them. ...Read more







