Health Advice
/Health

Hospital-acquired infections are rising – here’s how to protect yourself in health care settings
A new study from the National Institutes of Health shows a jump in both hospital-acquired infections and resistance to the antibiotics used to treat them. The findings are based on data gathered at 120 U.S. hospitals from January 2018 to December 2022, a five-year period that included the COVID-19 pandemic. Dr. Nasia Safdar, a professor of ...Read more

Researchers explore potential for AI to predict patients' pain management support needs after surgery
A Mayo Clinic retrospective study of 9,731 patients explored the potential of artificial intelligence (AI) to predict a patient's need for opioid refills after surgery. The study used deep learning models, a form of AI, to predict which patients are most likely to require additional opioid refills after surgery while ensuring adequate pain ...Read more

Women need more sleep than men do, studies say
It turns out there might be a scientific reason behind women needing extra “beauty sleep.” Studies show, on average, women require about 11 minutes more sleep per night than men do. Although this difference might seem small, it can have significant implications for overall health and well-being.
Research is limited, but the reasoning points...Read more

What you need to know about listeria
The Centers for Disease Control and Prevention has issued an alert after a listeria outbreak in several states. There have been at least two fatalities, and dozens have become sickened.
Dr. Nipunie Rajapakse, a Mayo Clinic pediatric infectious diseases expert, discusses the risks associated with listeria.
"Listeria is a type of bacteria that ...Read more

Plain ol' water is out. Hydration supplements are in. But do these top 8 brands really work?
You see them crowding checkout counters at grocery stores — a rainbow of bubble-gum pink, lime green and blueberry packets, slender and upright, like a multicolored chorus line of dancers tempting an impulse purchase. At the gym, they're dissolved into enormous jugs of cherry-tinted water.
They're especially prevalent on TikTok. Just search #...Read more
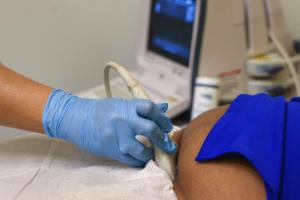
Women's health care is in a 'perilous place,' rankings say. Where does Florida stand?
MIAMI — Florida, with high numbers of uninsured and the lofty cost of care, ranks among the worst states in the country for women’s health, according to a new national report.
The Commonwealth Fund, a health care research nonprofit, ranked Florida 39th overall for women’s health and reproductive care in its 2024 scorecard, making it one ...Read more

Senate committee will subpoena Steward CEO, begin investigation into bankruptcy
Lawmakers in Washington D.C. say they are fed up with the Steward Health Care CEO’s refusal to volunteer information on what led to the medical system’s bankruptcy and the pending sale of its hospital properties, and so they will compel him to explain what occurred.
On Thursday, the U.S. Senate Committee on Health, Education, Labor and ...Read more

ADHD brains present unique challenges, but the condition is highly treatable − a primary care nurse practitioner with ADHD explains the science
“My brain has way too many tabs open.”
“Why can’t I complete tasks?”
“Why do I lose track of time?”
“Why can’t I pay attention?”
These are all things people with attention-deficit/hyperactivity disorder, or ADHD, may ask themselves daily, if not hourly.
As a healthandspirit/health/healthtips/s-3342843">Read more

New treatments offer much-needed hope for patients suffering from chronic pain
Hundreds of millions of people around the world experience chronic pain – meaning pain that lasts longer than three months. While the numbers vary from country to country, most studies estimate that about 10% of the global population is affected, so more than 800 million people.
The Centers for Disease Control and Prevention ...Read more

Mayo Clinic Minute: Dangers of heat-related illnesses
Prolonged exposure to both heat and humidity can lead to heat-related illnesses — from heat cramps to exhaustion to life-threatening heatstroke.
Dr. Jesse Bracamonte, a Mayo Clinic family physician, offers recommendations on what to do if you begin to feel ill.
Prolonged exposure to the heat and humidity can put you at risk for a range of ...Read more

Physicians' role crucial in using AI in patient care
Artificial intelligence is quickly transforming the health care landscape from helping to diagnose diseases to assisting in surgery. Its rapid progression has the potential to transform how health care teams work by streamlining processes and improving patient outcomes.
As AI is used more in health care, researchers stress that the technology ...Read more

What is laryngeal chondrosarcoma?
You may have heard about a recent first at Mayo Clinic, a total larynx transplant. What you may not have heard was what precipitated that transplant. The patient developed a rare form of cancer called laryngeal chondrosarcoma.
Dr. David Lott is a Mayo Clinic otolaryngologist who specializes in laryngeal cancer. He says your larynx, or voice box...Read more

COVID is surging again this summer in Maryland, hospitalization and wastewater data shows
BALTIMORE — Judging from local wastewater surveillance trends, President Joe Biden has plenty of company in Maryland as he continues to recover this week from his third bout of COVID-19.
The state is currently seeing the biggest spike in COVID levels in its wastewater — or sewage — since early January, according to data from the U.S. ...Read more

Can texting new parents to report their blood pressure help address maternal mortality? These doctors think so
PHILADELPHIA — Two Penn Medicine physicians had an unorthodox idea for reducing the number of patients who develop dangerously high blood pressure in the weeks after giving birth: Stop asking them to come into the doctor's office for blood pressure screenings.
Dangerously high blood pressure, is a leading cause of maternal death and hospital-...Read more

Oregon senator proposes criminal charges and fines for rogue Obamacare agents
Health insurance agents who fraudulently enroll consumers in Affordable Care Act health plans could be subject to criminal charges — and civil penalties of $10,000 to $200,000 — under legislation introduced Wednesday by Sen. Ron Wyden, D-Ore., chairman of the powerful Senate Finance Committee.
Wyden first promised the bill in May, when he ...Read more
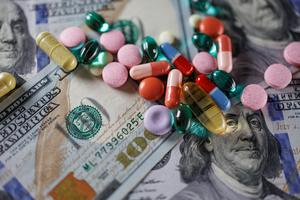
Cancer costs for Americans with private health insurance rose after the ACA rollout and fell for those with Medicaid
Low-income Americans ages 18 to 64 with cancer saved about US$1,250 per year on treatment within seven years of the 2014 rollout of the Affordable Care Act, according to my recent study.
Those patients either personally earned or were in families that made $17,609 or less per year and therefore were eligible for Medicaid, the ...Read more
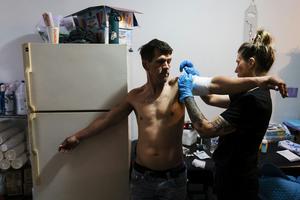
Xylazine wounds are a growing crisis among drug users in Philly − a nurse explains potential causes and proper treatment
Warning: This article contains graphic images.
Xylazine or “tranq” wounds – characterized by deep pockets of dead tissue – have become increasingly visible in Philadelphia among people who use drugs.
That’s because xylazine, an animal tranquilizer with no FDA-approved use in humans, is now pervasive in Philadelphia�...Read more

Environmental Nutrition: High fiber diet and CVD
Q: Can eating a diet high in fiber reduce my risk of developing cardiovascular disease?
A: Yes, several studies have linked high-fiber diets to a reduced risk of developing cardiovascular disease (CVD).
Current fiber recommendations are for women to consume 25 grams/day and for men to consume 38 grams/day. However, surveys show that a meager 5...Read more

These 6 veggies are as hydrating as they are healthy
Drinking plenty of fluids throughout the day is key to staying properly hydrated, but it’s not the only way to replenish your body’s water stores. In addition to keeping a filled water bottle on hand, there’s a variety of hydrating foods you can eat — especially fruits and vegetables — that are naturally full of water to help you meet ...Read more

Make virtual mental health care visits work for you
Before the pandemic, talking to a therapist or psychiatrist on a video call was novel. Now it’s fairly common. One recent analysis, for example, found that video appointments within the massive Veterans Affairs Health Care System jumped from about 2% of all mental health care encounters in January 2019 to 35% of these encounters in August 2023...Read more
Popular Stories
- New treatments offer much-needed hope for patients suffering from chronic pain
- Women need more sleep than men do, studies say
- Plain ol' water is out. Hydration supplements are in. But do these top 8 brands really work?
- What you need to know about listeria
- Researchers explore potential for AI to predict patients' pain management support needs after surgery





