COVID-19 can cause lasting lung damage – 3 ways long COVID patients' respiration can suffer
Published in Health & Fitness
“I just can’t do what I used to anymore.”
As pulmonologists and critical care doctors treating patients with lung disease, we have heard many of our patients recovering from COVID-19 tell us this even months after their initial diagnosis. Though they may have survived the most life-threatening phase of their illness, they have yet to return to their pre-COVID-19 baseline, struggling with activities ranging from strenuous exercise to doing laundry.
These lingering effects, called long COVID, have affected as many as 1 in 5 American adults diagnosed with COVID-19. Long COVID includes a wide range of symptoms such as brain fog, fatigue, cough and shortness of breath. These symptoms can result from damage to or malfunctioning of multiple organ systems, and understanding the causes of long COVID is a special research focus of the Biden-Harris administration.
Not all breathing problems are related to the lungs, but in many cases the lungs are affected. Looking at the lungs’ basic functions and how they can be affected by disease may help clarify what is on the horizon for some patients after a COVID-19 infection.
The main function of the lungs is to bring oxygen-rich air into the body and expel carbon dioxide. When air flows into the lungs, it is brought into close proximity with the blood, where oxygen diffuses into the body and carbon dioxide diffuses out.
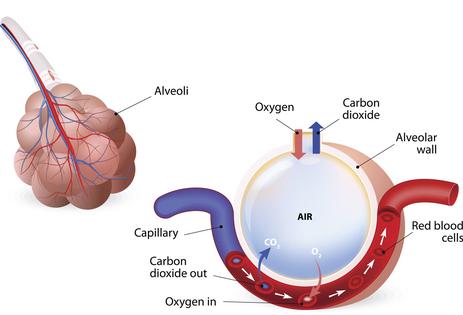
This process, as simple as it sounds, requires an extraordinary coordination of air flow, or ventilation, and blood flow, or perfusion. There are over 20 divisions in your airway, starting at the main windpipe, or the trachea, all the way out to the little balloons at end of the airway, called alveoli, that are in close contact with your blood vessels.
By the time a molecule of oxygen gets down to the end of the airway, there are about 300 million of these little alveoli it could end up in, with a total surface area of over 1,000 square feet (100 square meters) where gas exchange occurs.
Matching ventilation and perfusion rates is critical for basic lung function, and damage anywhere along the airway can lead to difficulty breathing in a number of ways.
One form of lung disease is obstruction of airflow in and out of the body.
Two common causes of impairments like these are chronic obstructive pulmonary disease and asthma. In these diseases, the airways become narrowed because of either damage from smoking, as is common in COPD, or allergic inflammation, as is common in asthma. In either case, patients experience difficulty blowing air out of their lungs.
...continued









Comments