Current News
/ArcaMax

Colorado CDL program for immigrant truckers indefinitely suspended
DENVER — Colorado’s program for issuing commercial driver licenses to immigrants with temporary legal status has been shut down for nearly two months and remains indefinitely suspended as state officials conduct an audit in response to a federal government crackdown on illegal trucking.
U.S. Transportation Secretary Sean Duffy has ordered ...Read more

Ghislaine Maxwell brings last-ditch bid to toss conviction, could impact release of 'Epstein files'
NEW YORK — Ghislaine Maxwell on Wednesday asked a federal court to throw out her sex trafficking conviction and 20-year prison sentence for aiding Jeffrey Epstein’s sexual exploitation of teenage girls.
In a habeas petition filed in Manhattan Federal Court, the former socialite — representing herself — argued new information arising...Read more

US core CPI eases to four-year low in shutdown-impacted report
Underlying U.S. inflation rose in November at the slowest annual pace since early 2021, an unexpected improvement in a report muddled by the government shutdown.
The core consumer price index, which excludes the often-volatile food and energy categories, increased 2.6% in November from a year ago, according to Bureau of Labor Statistics data ...Read more
Florida's new license plate law leads to immigration detention and a wrongful arrest in Broward County
FORT LAUDERDALE, Fla. — Justin Cuellar was driving through Davie with his father to pick up their trailer last Tuesday when a Florida Highway Patrol trooper knocked on their window.
He told them that it was difficult to see the “Sunshine” letters on their truck’s license plate and they couldn’t have anything obstructing it, Cuellar, ...Read more
Protesters ask judge to stop ICE from deleting messages about Charlotte arrests
CHARLOTTE, N.C. — A judge declined to rule on Wednesday whether federal agents must preserve text messages discussing the arrest of two protesters at a U.S. Department of Homeland Security office in Charlotte.
Magistrate Judge David Keesler gave Heather Morrow and William Stanley unsecured $25,000 bonds in the meantime. But he said he would ...Read more

Pope Leo XIV names Bishop Ronald Hicks as new archbishop of New York
Pope Leo XIV has announced fellow Chicagoan, Bishop Ronald Hicks of Joliet, Ill., will serve as the next archbishop of New York, replacing Cardinal Timothy Dolan, who has led the state’s 2.8 million Catholics for more than 15 years.
“I am grateful to Pope Leo for appointing such a splendid priest and bishop to serve you, and have pledged to...Read more

China seeks to mediate Thai-Cambodia border clash
China’s top diplomat held separate talks with his counterparts in Thailand and Cambodia as Beijing seeks to mediate a border clash after a new bout of violence between the two countries threatened to derail a ceasefire brokered by U.S. President Donald Trump.
Chinese Foreign Minister Wang Yi was briefed by envoys from Thailand and Cambodia ...Read more

Budget shortfall less than expected in Kentucky; Beshear to share reduction plan
LEXINGTON, Ky. — A group of economists predicts Kentucky will soon see a revenue shortfall, one that is about half of what they projected three months ago for the fiscal year ending June 30, 2026. From now until the middle of 2028, the state’s income will likely see shy, moderate growth, the economists said.
Optimistic, pessimistic and ...Read more

Mamdani, dozens of other pols press NYC hospitals to cut labor deal with nurses as deadline looms
NEW YORK — Mayor-elect Zohran Mamdani and more than 100 other local politicians are putting pressure on some of New York City’s largest private hospitals to settle a labor dispute with their unionized nurses before their contracts expire at the end of the year.
In an open letter shared exclusively with the Daily News on Wednesday, Mamdani ...Read more

Lead prosecutor in Bovino murder-for-hire case unexpectedly leaving US attorney's office ahead of trial
CHICAGO — The federal prosecutor who had been heading up a high-profile case alleging a Chicago gang member solicited the murder of Border Patrol chief Gregory Bovino is leaving the U.S. attorney’s office just weeks ahead of a scheduled trial.
Bradley Tucker, who joined the U.S. attorney’s office in June 2022 and had been assigned to the ...Read more

Florida Gov. Ron DeSantis called this Muslim group a foreign terrorist organization. They are suing
MIAMI — A Muslim civil rights group filed a lawsuit against Florida Gov. Ron DeSantis over his executive order last week that designated it and another organization as “foreign terrorist organizations,” arguing the move was unconstitutional and “discriminatory.”
The Council on American-Islamic Relations, known as CAIR, is a Muslim ...Read more
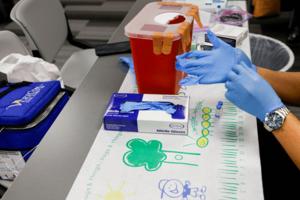
Florida vaccine debate: explaining chickenpox, Hep B, Hib and pneumococcus shots
MIAMI – Florida’s surgeon general wants to do away with all state vaccine mandates. But the first step in his plan targets four specific vaccines.
Earlier this month, the Department of Health had a meeting during which officials unveiled a proposal to drop the requirement for the chickenpox; the Hepatitis B; the Haemophilus influenzae type ...Read more

The Jeffrey Epstein files are finally set to be released. Here's what to know
After years of debate, investigations and conspiracy theories, the Department of Justice is scheduled on Friday to finally release the Jeffrey Epstein files.
The release will come nearly 20 years after federal prosecutors in the Southern District of Florida cut a remarkably lenient plea deal with Epstein that allowed him to avoid a lengthy ...Read more

Ukraine security plan offers robust protections, officials say
The U.S. and Ukraine’s European allies have put together a plan of security guarantees containing detailed, robust and serious measures to ensure that any peace deal with Russia holds, according to officials familiar with the proposals.
An 800,000-strong Ukrainian army would provide the first line of postwar deterrence, with weapons and other...Read more

Russia will be paying for its war on Ukraine long after it ends
Russia will be paying for its invasion of Ukraine for years to come even if the fighting ended tomorrow, as the government plugs a widening gap in the military budget with increasingly costly borrowing.
As U.S. President Donald Trump pushes for a deal to end the war, the future bill for Moscow keeps growing. In one of the final bond auctions ...Read more

LA Councilmember John Lee hit with $138,000 fine in Las Vegas gift case
LOS ANGELES — Los Angeles City Councilmember John Lee is facing a steep fine for his notorious 2017 trip to Las Vegas, with the city's Ethics Commission saying he must pay $138,424 in a case involving pricey meals and expensive nightclub "bottle service."
On Wednesday, the commission decided 4 to 0 that Lee, who represents the northwest San ...Read more

Illinois mom covers 250-mile distance to reunite formerly detained immigrants with their Chicago families: 'They deserve to know somebody cares'
It’s pitch-black and frigid in the parking lot of an Italian restaurant in Michigan City, Indiana, by the time a small group of volunteers and immigrants gather in a circle, arms resting on each other’s shoulders and heads bent in prayer.
A pastor tells three Chicago-area men, who just hours ago had been released from an ICE detention ...Read more

Missouri legalized abortion, but most residents can't get appointments and go elsewhere
ST. LOUIS — Over a year ago, Missouri voters approved enshrining abortion rights into the state constitution. Lawyers won court cases, blocking clinic restrictions. Providers promised that Missourians could access abortions close to home.
But today, appointments are hard to come by at the three Planned Parenthood clinics — in Kansas City, ...Read more

DACA was once a lifeline for undocumented youth. It's leaving the next generation behind
Alex immigrated to the U.S. as a toddler and has long felt haunted by his undocumented status.
In 2017, when he turned 15, he was finally old enough to apply for the Deferred Action for Childhood Arrivals program, only for it to slip from his grasp right before he started the paperwork, when it was rescinded by the Trump administration.
Then, ...Read more
Rising electric bills lead to state scrutiny -- but little relief for residents
The last time the Maine Public Utilities Commission considered an electricity price hike, the proposal received fewer than 90 comments from the public.
Three years later, amid skyrocketing energy prices, more than 800 people weighed in on the plan, showing up to public hearings and even protesting outside.
The commission last month ultimately ...Read more
Popular Stories
- Illinois mom covers 250-mile distance to reunite formerly detained immigrants with their Chicago families: 'They deserve to know somebody cares'
- Trump announces military 'warrior dividend' amid inflation woes
- Missouri legalized abortion, but most residents can't get appointments and go elsewhere
- DACA was once a lifeline for undocumented youth. It's leaving the next generation behind
- It's an open secret that some of Philadelphia's charter schools push out kids with behavioral problems, principals say





