People can have food sensitivities without noticeable symptoms – long-term consumption of food allergens may lead to behavior and mood changes
Published in Science & Technology News
The prevalence of food allergies is increasing worldwide, approaching an epidemic level in some regions. In the U.S. alone, approximately 10% of children and adults suffer from food allergies, with allergies to cow’s milk, eggs, peanuts and tree nuts being the most common. Some patients have mild symptoms that might not need medical attention, leaving these cases unreported.
Food allergies, or food hypersensitivities, result from the overreaction of the immune system to typically harmless proteins in food. They can manifest as a spectrum of symptoms, ranging from itching, redness and swelling for milder reactions, to vomiting, diarrhea, difficulty breathing and other potentially life-threatening symptoms for severe reactions.
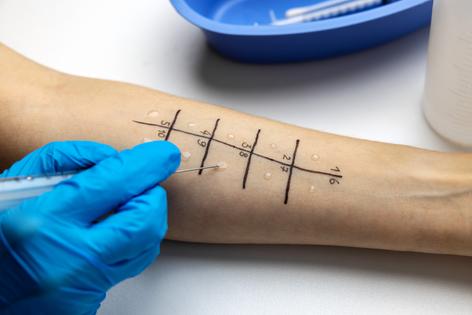
Besides self-reporting, food allergies can be diagnosed by exposing patients to trace amounts of offending proteins, or allergens, via their mouth or skin and observing their immediate reactions. More commonly, doctors use blood tests to measure the levels of immunoglobulin E, or IgE, a specialized antibody that the immune system uses to identify allergens and trigger a response. Although healthy individuals may have low levels of IgE in the blood, patients with food allergies have much higher levels that increase their risk of having severe allergic reactions.
But some people who test positive on skin-prick allergy tests with moderate increases in IgE don’t notice any allergy-related symptoms when they eat the allergen. This condition is sometimes referred to as asymptomatic sensitization. In many cases, people with this condition may not even be aware that they have a food hypersensitivity.
Are they truly asymptomatic, though? Or are there effects within their body that they aren’t aware of?
I am a neuroscientist studying how the brain is affected by food allergies. I became interested in this topic when I found that some of my family members had a hypersensitivity to cow’s milk. Some totally avoid dairy products because they have experienced severe, life-threatening symptoms. Those who don’t have typical allergic reactions occasionally eat dairy, but appear to develop seemingly unrelated illnesses a day or two later.
What I and other researchers have found is that food allergens can affect your brain and behavior if you’re hypersensitized, even if you don’t have typical food allergy symptoms.
Researchers have suspected food hypersensitivities to be a potential cause for behavioral disorders for decades.
A 1949 case report described behavioral and mood disturbances in patients after they ate certain foods, such as milk and eggs. Their symptoms improved after removing the suspected foods from their diet, suggesting that a food hypersensitivity was the likely culprit. However, I was intrigued that the patients had been able to eat the offending foods up until they chose to avoid them. In other words, they were asymptomatically sensitized, or tolerant, to the allergens.
Several recent studies in people have supported the association between food allergies and various neuropsychiatric disorders, including depression, anxiety, attention-deficit/hyperactivity disorder and autism. They strengthen the possibility that some reactions to food allergens could involve the nervous system and manifest as behavioral disorders.
However, the idea of food hypersensitivity causing neuropsychiatric disorders is still controversial because of inconsistencies across studies. Differences in the types of allergies, ethnic backgrounds, dietary habits and other factors among the study participants can produce conflicting results. More importantly, some studies included those with self-reported food allergies, while others included only those with lab-confirmed food allergies. This limited investigations to only symptomatic individuals.
My laboratory tested whether food allergens could manifest as behavioral symptoms, particularly in asymptomatically sensitized individuals. We wanted to find out whether eating offending foods could lead to brain inflammation and behavioral changes after sensitization, even in the absence of other obvious severe reactions.
To minimize the individual differences found in human studies, we decided to work with mice. We sensitized mice of the same age and genetic background to the common milk allergen β-lactoglobulin, or BLG, and fed them the same diet in the same room. We found that while BLG-sensitized mice produced moderately but significantly elevated levels of IgE, they did not show immediate allergic reactions. They could even eat food containing the milk allergen for two weeks without showing any obvious symptoms, despite maintaining elevated levels of IgE. This indicated that they were asymptomatically sensitized.
We then observed whether they showed any changes in emotionally driven behavior. Because we could not ask mice how they felt, we deduced their “feelings” by noting changes from their normal, survival-oriented behavior. Mice instinctively explore their environment to search for food and shelter while avoiding potential danger. However, “anxious” mice tend to spend more time hiding to play it safe. We identified “depressed” mice by briefly holding them by the tail. Most mice will keep fighting to get out of the uncomfortable predicament, while depressed mice quickly give up.
Our experiments were designed to simulate situations where asymptomatically sensitized individuals would eat either a large amount of an offending food in one day or small amounts every day for a few weeks. We mimicked these situations by placing a large amount of the milk allergen directly into the stomach of sensitized mice with a feeding tube, or giving them an allergen-containing mouse chow to eat the allergen a little at a time.
Interestingly, BLG-sensitized mice showed anxiety-like behavior one day after receiving a large amount of the allergen. Another group of sensitized mice developed depression-like behavior after eating small amounts of allergen for two weeks. In addition, BLG-sensitized mice showed signs of brain inflammation and neuronal damage, suggesting that changes in the brain may be responsible for their behavioral symptoms.
We also investigated the long-term effect of allergen consumption by keeping BLG-sensitized mice on the allergen-containing diet for one month. We found that IgE levels declined in sensitized mice by the end of the month, indicating that continually eating small amounts of the allergen led to decreased immune responses, or “desensitization.” In contrast, signs of brain inflammation remained, suggesting that the harmful effect of allergens persisted in the brain.
Researchers have yet to study prolonged brain inflammation, or neuroinflammation, in people who are asymptomatically sensitized. In general, though, chronic neuroinflammation is a known contributor to neurodegenerative diseases, such as multiple sclerosis and Alzheimer’s disease, although the exact causes of these diseases are unknown. A better understanding of the role allergens play in neuroinflammation can help researchers clarify whether food allergens trigger chronic inflammation that can lead to these diseases.
This knowledge could be especially important for patients undergoing oral immunotherapy, an approach to allergy treatment that involves incrementally ingesting small amounts of allergens over time. The goal is to desensitize the immune system and reduce the incidence of anaphylaxis, or life-threatening allergic reactions. In 2020, the U.S. Food and Drug Administration approved a standardized form of peanut allergens to prevent anaphylaxis in eligible pediatric patients. However, its possible long-term effect on the nervous system is unknown.
Food allergens can affect the brain and behavior of seemingly asymptomatic people, making them not so asymptomatic neurologically. Considering how your brain responds to the food you eat puts a whole new meaning to the phrase “you are what you eat.”
This article is republished from The Conversation, an independent nonprofit news site dedicated to sharing ideas from academic experts. It was written by: Kumi Nagamoto-Combs, University of North Dakota. Like this article? subscribe to our weekly newsletter.
Read more:
Harnessing the brain’s immune cells to stave off Alzheimer’s and other neurodegenerative diseases
Shorter days affect the mood of millions of Americans – a nutritional neuroscientist offers tips on how to avoid the winter blues
Kumi Nagamoto-Combs receives funding from the National Institute of Allergy and Infectious Disease and the National Institute on Aging.










Comments