HIV self-test kits are meant to empower those at risk − but they don't necessarily lead to starting HIV treatment or prevention
Published in Health & Fitness
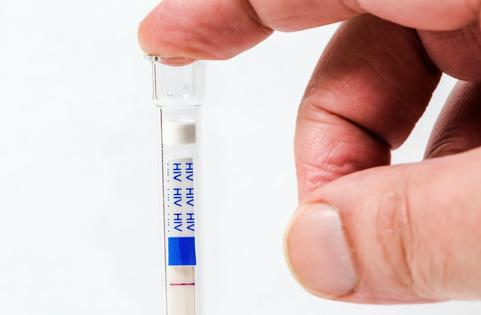
HIV self-test kits were developed to make it easier for people to access HIV testing. However, our research team has found that many people who use self-test kits do not go on to receive needed HIV treatment or start preexposure prophylaxis, or PrEP, to prevent future infection.
In 2016, the World Health Organization recommended HIV self-test kits as a way for people to confidentially test for HIV in their homes or other private places. Each kit contains detailed instructions on how to administer the test and read the results without the help of a clinician. However, the instructions advise confirming results in a health facility to improve access to care, especially for those with a positive reading.
Our team conducted a systematic review and meta-analysis of published research and data to understand how HIV self-testing influences access to HIV care and sexual behavior. Specifically, we looked at whether a positive test result led someone to seek care in a hospital or health facility to start treatment and whether a negative test result led someone at risk of contracting HIV to take preventive measures. We also looked at whether test results affected the number of sexual partners, engagement in anal sex without a condom and frequency of condom use.
Based on the 15 studies that met our criteria, we found that while HIV self-testing increased a person’s chances of finding an HIV clinic or doctor by 8%, many people did not initiate HIV treatment or PrEP following self-testing.
Female sex workers who used HIV self-test kits were 47% more likely to seek medical care, but this did not reduce the number of clients they saw per night.
For men who have sex with men, using HIV self-test kits may have increased the amount of condomless anal sex they have, according to one U.S. study. Those who use HIV self-test kits were more likely to have condomless anal sex with HIV-positive and HIV-negative partners, as reported by one Chinese study.
Many people are living with HIV and receiving treatment. However, some HIV-positive people are unaware of their HIV status and are at risk of infecting other people. Routinely checking your HIV status is important to prevent the spread of HIV.
Unfortunately, HIV testing is low in many regions of the world. Researchers from South Africa, the Netherlands and the United States have reported a lack of HIV testing among different parts of the population, including men who have sex with men. There are many barriers to HIV testing, including lack of knowledge about HIV and fear of stigma and discrimination.
Despite the availability of HIV test kits, many people at heightened risk have never been tested for HIV. As our research shows, some of those who test positive don’t receive treatment. Nor do all those who test negative but are at risk of infection receive preventive treatment or change their sexual behavior.
We found only one study that looked at how HIV self-testing influences PrEP use among men who have sex with men.
More research is needed to better understand the link between HIV self-testing and HIV prevention.
Our next step is to understand why people did or did not receive care following HIV self-testing. We plan on interviewing HIV self-test kit users about their experience using the self-test and whether they went on to receive care.
We hope the results of this study will help us build an intervention to increase access to care following an HIV self-test. This will contribute toward the national plan to end the HIV epidemic by 2030 in the U.S.
The Research Brief is a short take on interesting academic work.
This article is republished from The Conversation, an independent nonprofit news site dedicated to sharing ideas from academic experts. If you found it interesting, you could subscribe to our weekly newsletter.
Read more:
Use of HIV prevention treatments is very low among Southern Black gay men
Handkerchief or tissue? Which one’s better for our health and the planet?
Adeagbo Oluwafemi Atanda receives funding from University of Iowa and National Institutes of Health.
Engelbert Bain Luchuo and Oluwaseun Abdulganiyu Badru do not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and have disclosed no relevant affiliations beyond their academic appointment.









Comments