Parents
/Home & Leisure

Indoctrination and gender ideology: A look at Moms for Liberty's claims about NC schools
RALEIGH, N.C. — National and local leaders of Moms for Liberty came to Raleigh this week to promote a message that parents have to fight against indoctrination of their children by public schools.
Panelists at the Town Hall voiced concerns on issues such as a rise in school crime and teacher turnover and the difficulties of parents getting ...Read more

Lori Borgman: Took the bait, hook, line and sinker
I took the bait and I'm not even embarrassed to say what the bait was.
It was a fishing scam. Not trout, bass, anything you throw back in the water, or cook on the grill -- fishing with a "ph." Phishing.
Phishing is when online fraudsters try to scam you out of money by enticing you to open an email or text without first checking the web ...Read more

Rockstar’s vulnerable, transformative journey from debauchery to redemption
The subtitle for Ben Mason’s memoir "Sex, Trucks, and Rock ‘N Roll" is “a Spiritual Journey,” but that’s much too tidy for this book. “ It’s four in the morning,” starts chapter one, “ and I’m still wired.”
So starts this headstrong story of the life of a musician, songwriter and free-thinking drummer. Every girl wants to ...Read more
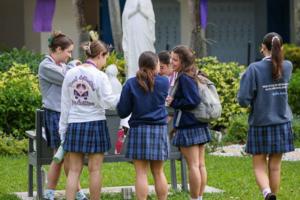
The voucher effect? South Florida Catholic schools see more kids, even waiting lists
MIAMI -- Helped by an influx of new Floridians, and boosted by the state’s newly expanded voucher system, Catholic schools in South Florida are seeing steady growth and even adding new classrooms. That’s in stark contrast to what’s going on in the public schools, particularly in Broward County, which faces tough decisions on closing entire...Read more

Lori Borgman: Conversations are growing ear-resistible
My husband and I have experienced some hearing loss. The most frequently heard word at our house is "WHAT!?"
More pressing than our physical hearing loss is our selective hearing loss, something that happens to couples who have been married a long time.
Just the other day, the husband was working on his laptop at the kitchen table with his ...Read more

Bright outdoor light at night may increase stroke risk
Too much exposure to bright outdoor lights at night may increase a person's stroke risk, new research suggests.
The study involved more than 28,000 people living in a large city in China. Researchers found that people exposed to the highest levels of artificial outdoor light at night had a 43% increased risk of developing cerebrovascular ...Read more

A call to compassion and understanding in an increasingly divided world
Set against the backdrop of post-Roe v. Wade America, "Refuge" by Bill VanPatten dives into the profound impact of state laws on individual freedoms and explores the complexities of family, prejudice, and resilience in the face of adversity, all while fearlessly delving into the intricacies of a woman’s right to choose.
Jesse Pérez, who is ...Read more

Strokes in young adults may be caused more often by migraines, other nontraditional factors
Strokes are typically caused by high blood pressure and other traditional risk factors. But for adults under 35 who have a stroke, migraine headaches and other nontraditional risk factors may be more likely to blame, new research finds.
The higher risk declines as people age, according to the study, published in the American Heart Association ...Read more

She survived a cardiac arrest. Her husband didn't
Danielle McCollian needed some work done at her house. While at the post office, she saw an ad on the bulletin board for a guy who did remodeling.
She called, he came out and that was that. They married when she was 39 and Joe was 32. A year later, they decided to start a family. After several miscarriages, she used in vitro fertilization to ...Read more

Lori Borgman: You make the call: Take the phone or leave it
I left home without my phone the other day. I considered turning back but decided against it.
As I continued on my way, I felt a growing sense of euphoria. It was as though a weight had been lifted -- a small electronic weight that would fit in a pocket, a purse or rattle around in a cup holder in a car. It was freeing. For a short distance ...Read more

Women with pregnancy complications may be able to lower future cardiovascular risk
Women with a history of pregnancy complications are at higher risk for cardiovascular disease, but they can greatly lower that risk, new research suggests.
Having healthy lifestyle behaviors and managing blood pressure, cholesterol and blood glucose levels after giving birth significantly lowered their risk for future cardiovascular disease to ...Read more

Can these child care centers survive? What their fight means for parents, employers
BOISE, Idaho — Boise City Council Member Luci Willits was a junior in college when she had her first child.
At the time, she and her husband couldn’t afford child care. Instead, they planned their class schedules so that one of them was always available to take care of the baby. Occasionally, in a pinch, Willits had to bring her daughter ...Read more

Emotionally charged novel reflects on mortality, loss and redemption
Maybe it’s that I’m at an age where I ponder mortality more than others. Regardless, "The Rainbow Diary," a novel by Mitch Maiman, hit an emotional nerve and had me thinking long and hard about his truly intelligent and insightful protagonist, his story and the message he delivers about one of our greatest mysteries.
Readers get a sense of ...Read more

Debra-Lynn B. Hook: Southern-born transplant to Ohio marvels: Isn't Easter supposed to be pretty?
Growing up and then living in the Deep South for years as I did, Easter was synonymous with azaleas, temperatures in the 70s and children skipping through new spring grass looking for colored eggs.
Easter came in the spring, after all.
You know: Sunshine. Green trees. Bunnies, hopping down the bunny trail.
And then I moved to the tundra, aka ...Read more

Lori Borgman: Bigger house and fewer kids don't mean more closet space
We began married life in a 1930s Craftsman bungalow with three small bedrooms. Each bedroom had a closet the size of a telephone booth. Everything fit.
We added a baby to the mix. Everything fit.
We added a second and third baby. Everything fit.
Today, we live in a four-bedroom house with double-wide closets in every bedroom and a small walk-...Read more

What is luminal B cancer, the condition Olivia Munn suffers from?
Olivia Munn shared a gallery of photos and video on social media recently, revealing she was diagnosed with breast cancer. The actress thanked her family and friends for their support, while providing a detailed explanation of how she became diagnosed.
“I tested negative for all, including BRCA (the most well-known breast cancer gene). My ...Read more
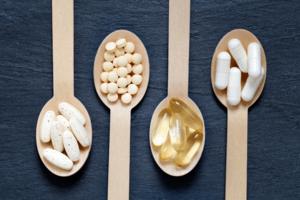
What a researcher takes for healthy aging, and the risks involved
University of Arizona professor Cynthia Thomson is a dietician and cancer prevention expert. She’s run marathons, battled colorectal cancer and extensively studied the health benefits of the supplements she takes to encourage healthy aging.
Although her research has shown there are risks attached, she takes vitamin D and calcium supplements ...Read more

Sci-fi thriller reveals unprecedented medical breakthrough that stops death in its tracks
Is death really inevitable? That’s the fascinating premise of this unique novel — part science fiction fantasy, part medical thriller, part romance — about a gifted ER doctor who is so devastated by seeing his patients dying that he comes up with a mind-boggling theory for “curing death.”
Just like medicine can be used to save people ...Read more

Debra-Lynn B. Hook: The personal and universal of modern loneliness
Two friends take turns on alternating mornings making eggs and toast for me.
They straighten my bed, wash my linens and take out the trash.
They go to the grocery store, fill the bird feeder, water the plants and make lunch and enough food for dinner.
They talk and laugh and share life with me, from 9 to 3.
At which point I am alone.
For ...Read more

Lori Borgman: Forgiving and forgetting, the hardest thing you may ever do
My grandma used to say she could forgive, but she couldn't forget. This was always in reference to a comment made by a neighbor about pickles my grandmother had entered at the fair. The neighbor criticized the pickles for being sliced as rounds instead of spears, or maybe it was the other way around.
Grandma was a good woman. Hard worker. ...Read more





